Simulation Centres
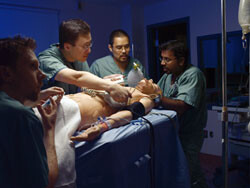
The Department of Anesthesia established the first program in Canada to incorporate simulation-based technology in medical education. To date, three of the centres (St Michael’s Hospital, Sunnybrook Health Sciences Centre and Hospital for Sick Children) are accredited by the Royal College of Physicians and Surgeons of Canada, and therefore are nationally recognized as leaders in simulation-based learning and educational research.
Simulation-based education is available to learners of all levels including undergraduate and postgraduate trainees and for continuing medical education. Single profession and interprofessional activities in collaboration with multidisciplinary teams can target a variety of objectives that allow for learning and consolidation of knowledge, skills and teamwork behaviour necessary for the practice of anesthesia. Simulation sessions are not limited to the laboratories at each of the teaching hospitals. In situ simulation, workshops at conferences, and an outreach program are also conducted. The whole spectrum of simulation modalities are included in our activities and innovation is prominent to meet the needs of advances in medical education. We partner with other groups within the University of Toronto community as well as local and international organizations.
The Royal College of Physicians and Surgeons of Canada is moving towards incorporating simulation-based milestone assessments in evaluating a trainee anesthesiologist’s readiness for independent practice. The University of Toronto Simulation program prepares candidates for these assessments and hosts the nationally standardized assessment sessions locally.
Electives and fellowships in simulation and medical education are offered at St Michael’s Hospital,Sunnybrook Health Sciences Centre, Mount Sinai Hospital and the Hospital for Sick Children. Research activities are prominent. For further information about simulation in the Department of Anesthesia at the University of Toronto, please contact Dr. Tobias Everett.
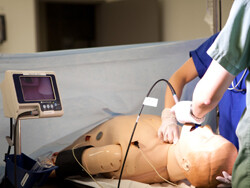
Sunnybrook Health Sciences Centre
The Sunnybrook Canadian Simulation Centre was the first simulation centre in Canada when it opened in 1994 and shortly thereafter pioneered the use of high fidelity simulation for undergraduate medical education in Canada. It is a multidisciplinary program, with attendees from many areas of healthcare including physicians, dentists, surgeons, nurses, respiratory therapists and others. There are active teaching programs, and every third year medical student at University of Toronto attends the Centre for two days ("Entry and Exit Sim") during their anesthesia rotation. There is also an active research program, with grants obtained from many funding agencies including CIHR and publications in high quality journals. The resources include high and low fidelity human patient mannequins, and in 2013 additional space was added to accommodate procedural skills education including basic and advanced techniques in minimally invasive surgery. Simulation activities occur within the Centre, as well as elsewhere at Sunnybrook using in situ simulation.
Women’s College Hospital
At Women’s College Hospital we have been running in situ high-fidelity simulation training for our multidisciplinary operating room teams managing critical events. We have simulated eight of the twelve critical events described by Ziewacz¹ including: 1. PEA arrest; 2. Tension pneumothorax; 3. Unstable bradycardia; 4. Unstable tachycardia; 5. MH crisis; 6. Anaphylaxis; 7. Fire in the OR; and 8. CO2/Air Embolus. We are interested in whether the use of Critical Event Checklists developed by Ziewacz improve the team’s adherence to key management points for these events. The debriefing has focused on non-technical skills such as teamwork and communication as well as points specifically brought to light during the simulations.
The simulation centre at Women’s College Hospital is also home to many part-task simulators and is used in the surgical training program for arthroscopic simulation.
¹ZiewaczJE, Arriaga AF, Bader AM, Berry WR, Edmondson L, Wong JM, Lipsitz SR, HepnerDL, Peyre S, Nelson S, Boorman DJ, Smink DS, Ashley SW, Gawande AA: Crisis Checklists for the Operating Room: Development and Pilot Testing. J Am CollSurg 2011; 213(2): 212-9
St Michael’s Hospital
Our structured Crisis Resource Management program has been incorporated into the core curriculum for all Anesthesia PGY 1-4s. It is held on Monday afternoons for four residents at a time. Residents are scheduled to attend sessions in the Allan Waters Patient Simulation Centre at the Li Ka Shing Knowledge Institute at St. Michael's Hospital (for which they are excused from their clinical duties). This program focuses on the management of common and rare anesthesia emergencies that may or may not be encountered during clinical training. It also focuses heavily on practicing non-medical skills related to Crisis Resource Management such as Communication, Situational Awareness, and Leadership. This environment offers a unique opportunity to be the primary anesthesiologist in an emergency as a trainee and better prepared for these emergencies as a consultant.
UHN – Toronto Western Hospital
The simulation laboratory at the Toronto Western Hospital is situated on the fifth floor in the McLaughlin Wing. At present we share the space with General Surgery. Our simulation lab contains part task trainers for both upper and lower limb peripheral nerve blockade. These models can be used to teach interscalene and supraclavicular brachial plexus blocks and also femoral nerve block. Each upper limb model is equipped with software that allows the user to learn which nerve they are targeting and provides a lecture series on the anatomy of the brachial plexus. The software provides an objective assessment when evaluating students doing simulated nerve blocks. In addition to regional anesthesia we also have part task trainers for teaching the management of a difficult airway. There are mannequins and assortment of equipment to perform tracheal intubation using laryngoscope, bronchoscope, through supraglottic airways, and surgical airway. There is also a high fidelity bronchoscopy simulator, AccuTouch. Residents and fellows who are interested in learning these skills have access to the laboratory during weekdays. We also have a dedicated Tuesday afternoon where we have an anesthesia assistant accompany the trainees for an afternoon in simulation training.
UHN – Toronto General Hospital
Toronto General Hospital offers teaching with high fidelity simulation on Tuesday mornings as trouble rounds. The residents are expected to manage anesthetic emergencies which is followed by debriefing. These cases consist of a wide range of adult anesthetic topics that are generally based on real life crisis situations. This form of teaching has been highly engaging and helps consolidate the knowledge and skills required for anesthetic practice.
Hospital for Sick Children
The Hospital for Sick Children is one of the international sites that offer the Managing Emergencies in Paediatric Anaesthesia (MEPA) course to their trainees in pediatric anesthesia. In addition, numerous interprofessional in situ simulation sessions are conducted in various locations in the hospital (including satellite anesthesia locations, trauma room, the Cardiac Diagnostic Interventional Unit, the operating room and the Post Anesthesia Care Unit) with the focus on teamwork skills. Pediatric focused simulation electives and fellowships are available through the Learning Institute at the Hospital for Sick Children.
Mount Sinai Hospital - SimSinai Centre
SimSinai Centre has three simulation rooms and one mock operating room. The centre is currently being used by many specialties including anesthesia, internal medicine, critical care, emergency medicine and obstetrics. As one of the major hospitals in maternal health and obstetrical anesthesia, training in maternal and neonatal crisis management can be performed on Noelle, the obstetric mannequin, and the wireless neonatal mannequin. In addition, in situ simulations of mega-codes are being conducted throughout the hospital with a focus on multi-disciplinary team work and identifying system errors. Various airway crisis scenarios are being conducted for the PGY 1-4 anesthesia residents. Moreover, the PGY2 residents receive further training in obstetrical anesthesia crisis management.